“If you need anything for pain, please let me know. Make sure you keep lying flat, and don’t move your leg Sir. If there is anything you need, I’ll be right outside.” I said pleased with a successful, stress-free admission of a fresh Cardiac Patient with 2 stents. A young man with no health history, aside from being a frequent smoker, admitted for what he thought was stomach upset and indigestion has just has his world rocked, his life saved, and his heart opened by the miracles of modern medicine. The admission assessment completed, he was still in a daze of Versed as he laid with the knowledge of his heart attack and life-saving interventions.
“I’m fine. Thank you”, he said, as I walked the 10 steps from his bed outside the door.
“OH SHIT. BED 6 is in V-FIB”.
I pause in my transition from standing to sitting. “What?” The words didn’t compute to me. “Bed 6?”, I thought, “Why does that sound so familiar to me?” “Why is this lady running in my patients room in a frenzy?”
After what seemed like an eternity of puzzlement on my behalf, I realized by the term Bed 6 sounded so familiar to me. It was my patient. My fresh cath, heart was quivering, he was unresponsive and his eyes were rolled back in his head.
“SOMEBODY THUMP HIM”, the nurse yelled, as she turned around and started to leave the room. “OH SHIT, GET THE CODE CART.” She stopped, turned around and took her petite right hand, clenched it tightly, and with passion and knowhow, forcefully placed it directly in the center of his chest. His heart reacted, for a few seconds the beats appeared to stabilize, and then again, V-Fib.
“You call that a thump?” An dry, witty nurse steps in, and amidst laughter and the occasional profanity the ballet that is a Code Blue in the CCU began to play out in front of me. These nurses stepped in, stepped up, and did what they do best.
The new nurse jumped up with her knees on the bed, someone pressed the CPR release on the bed, and it went flat. The nurse held on like a rodeo star, and in less than 8 seconds, another strong thump to the heart with given. Only this time, the adrenaline was in full force, and this nurse gave it gusto. Again, his heart rhythm appeared to stabilize,and for a few moments mine as well.
Then, V-Fib.
“Lets shock him!” Without even batting an eye, the pads were placed on the patient, “EVERYONE CLEAR?” The familiar sound of charging I hear the daily, when the equipment is tested. And Then a very new and different sound as 200 joules of electricity surge through the machine and into the patient and the patient nearly leaping off the bed, yelling, and grabbing his chest, as his heart is told to beat differently. His eyes bulged in his head. He looked like he might vomit, might punch someone in the face, and then, nearly as soon as it began, he lied peacefully. He converted. Heart rate 130’s, A fib.
“What’s all this?” He calmly asked as all eyes were on him. The room filled with nurses hanging on his every quazi-stable heartbeat, breath, and now : words. Surely every ounce of oxygen evaporated form the room in the seconds that followed, as everyone released the breaths that had been held and refilled their lungs. Laugher, praise, and relief were present in this tiny room. The patient even laughed as the nurses explained what had happened, he thanked them, laughed a bit himself, and went back to sleep.
But still there was the A-Fib.
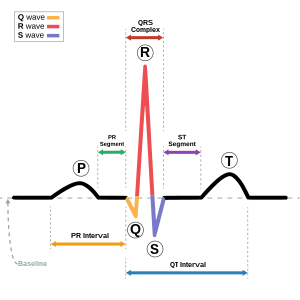 Image via Wikipedia
Image via WikipediaA quick call to the DOC, who is apparently a colorful fellow, often entitled and self-righteous, but talented and competent, and we had our orders. “You shocked him into it, now shock him back out”.
And that is exactly what they did. This time, since my own rhythm had converted, I actually participated, rather than looking dumb-founded. I documented, with precise times, accurate details, and beautifully accurate and legal nursing language.
1mg of Versed and 200 joules later, another leap off the bed, grab the chest, and yellow from the patient and there it was on the monitor: Sinus rhythm 64.
Beautiful.
Never in my life did I think I could call a heart rhythm beautiful, but no other words would be appropriate.
Again relief, though naturally, with less people, less fan-fair, and in an almost expected manner. He once again laughed slightly, thanked us, and went to sleep.
I assessed the patient. Everything was as it should be and had I not witnessed it with my own eyes, I would have never guessed the events that had just occurred.
Even with all the leaping, and excitement, the sheath in the groin remain intact, soft, no bleeding, no hematoma. The patient was stable, pain free, and safe.
They did it. We did it, in whatever small way my warm body contributed to this affair.
A mans life was saved 3 times that day, and it was routine for them, second nature, a part of the the job. patient was alive, doing well, standards and protocols were followed, and it was just another day in the Cardiac Critical care unit, only this day, I was a part of it.
To describe the seamless response of the Cardiac Care Unit to a heart emergency is difficult. I can think of no better way to paint an image for you than of a beautifully choreography ballet of hands, minds, and instinct. The fact that saving lives is second nature to them is inspiring and humbling. I’m thankful these nurses exist and am thankful for the opportunities I have to learn from them.
Download Nurse Bingo Today!

Liven up any shift with a fun game of bingo. See who can fill a row first!
Fill a whole card and lose grip with reality.
Your privacy is protected. We will never spam you.





I stopped reading when you noted that the nurses did not one, but two precordial thumps. Someone needs an ACLS refresher. Precordial thumps are for very specific cases: witnessed conversion to VT or pulseless VT when a defibrillator is NOT readily available. A cardiac CCU should definitely have a defib available. Just because we see the pretend doctors on TV doing it in every case of CPR doesn’t mean that we should follow suit. 🙂
The first “thump” really was just a tap. The reason the other nurse did the 2nd one was because the 1st one was too timid to do it “right”. Not sure if I wrote that clearly, but the first nurse really just tap him. She was a younger nurse, and apparently didn’t have the gaul to do a real thump like the more seasoned nurse.
Hi Webmaster,
Today i have visit on your web-blog first time and it is amazing and very informative, please keep it up..
God Bless You!!!
Thanks,
Dave
http://myhealthteacher.blogspot.com/
nah, I just got pulled there, but the next day I did hear some Afib in a patient on the floor and got them on telemetry! So a little rubbed off 🙂
So because of my computer problems, I may have missed that you have moved to the cardiac unit? You will definitely get more action there! Isn't it beautiful when things go as they should? Being an EMT, I zap people often but I still get all warm and fuzzy when the heart actually accepts the shock! It is more often the case that we shock V-Fib into asystole! Congrats on being a part of it and before you know it, you will be running for the crash cart like it was second nature!!
Very nice information please keep it up